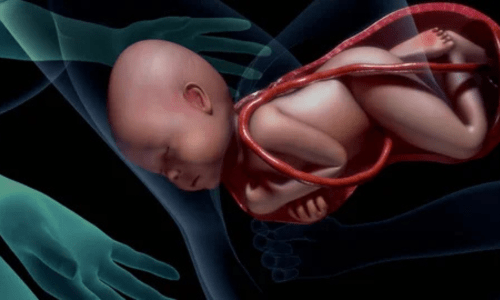
Vaginal Delivery: A Natural and Empowering Birth Experience
Vaginal delivery, also known as normal delivery, remains the most common and preferred method of childbirth worldwide. It involves the baby passing through the birth canal naturally, guided by the mother’s contractions and pushing efforts. For low-risk pregnancies, healthcare experts often recommend attempting vaginal birth due to its numerous advantages for both mother and baby.
What Happens During Vaginal Delivery?
The process unfolds in three main stages.
The first stage begins with labor contractions that cause the cervix to thin (efface) and dilate up to 10 cm. This phase can last several hours or even a day for first-time mothers, transitioning from early mild contractions to stronger, more frequent active labor. Pain management options like breathing techniques, epidurals, or hydrotherapy help many women cope.
The second stage is the pushing phase, where the mother actively bears down with contractions to guide the baby through the vagina. This culminates in the birth of the baby, often with the head emerging first (crowning), followed by the shoulders and body.
The third stage involves delivering the placenta, which usually occurs within 5–30 minutes after the baby arrives.
Throughout, medical support monitors the baby’s heart rate and the mother’s progress to ensure safety.
Benefits of Vaginal Delivery
Vaginal birth offers significant advantages over cesarean sections in uncomplicated cases. Mothers typically experience quicker recovery, often returning to daily activities within days rather than weeks. Hospital stays are shorter, with lower risks of surgical complications like infections, excessive bleeding, or blood clots.
For the baby, passing through the birth canal exposes them to beneficial maternal bacteria, which supports immune system development and may reduce long-term risks of conditions like asthma or allergies (per the hygiene hypothesis). Babies born vaginally also tend to have fewer immediate respiratory issues compared to those delivered by C-section.
Additionally, vaginal delivery promotes early bonding through immediate skin-to-skin contact and can facilitate breastfeeding initiation. It avoids abdominal surgery scars and anesthesia-related effects, making it a more natural process that empowers many women.
Potential Risks and Considerations
While generally safe, vaginal delivery carries some challenges. Labor can be intense and painful, with risks of perineal tearing, episiotomy, or pelvic floor strain leading to temporary issues like urinary incontinence. In rare cases, labor may not progress, requiring interventions like forceps, vacuum assistance, or emergency cesarean.
High-risk factors—such as breech position, placenta previa, or certain maternal health conditions—may make cesarean safer. Always discuss options with your obstetrician for personalized guidance.
In summary, vaginal delivery promotes faster healing, better microbial seeding for the newborn, and a fulfilling birth journey when conditions allow. With proper prenatal care and support, it remains a safe, empowering choice for most expectant mothers.
